SO. HUNTER ALEXANDER: THE “GOLDEN WINDOW” UPDATE
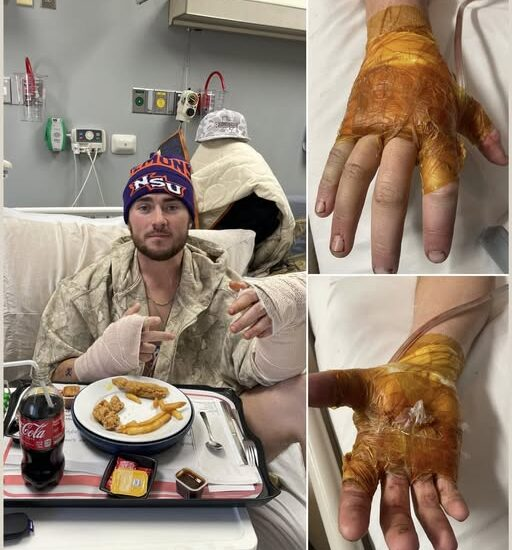
Latest Update on Hunter Alexander: ICU Red Alerts Signal Critical “Golden Window” in Recovery
Overnight, a surge of red alerts echoed through Hunter Alexander’s ICU room.
Monitors flashed. Alarms signaled change. Nurses moved quickly.
Doctors now describe this phase as a critical “golden window” — a narrow, high-stakes period where swift intervention can protect hard-won surgical progress… or where small shifts can escalate into major setbacks.
For Hunter, who is recovering from complex electrical trauma and multiple surgeries, the margin is razor thin.
What Happened Overnight?
According to medical staff, Hunter experienced:
- Rapidly rising fluid levels
- Intense, persistent muscle spasms
- Elevated inflammation indicators
For most patients, fluid fluctuations can be manageable.
But in cases involving electrical trauma and repeated surgical reconstruction, rising fluids are not routine. They can signal:
- Circulatory stress
- Compartment pressure elevation
- Systemic inflammatory response
- Early warning signs of infection
Electrical injuries travel deeper than surface burns. They damage muscle fibers, blood vessels, and nerves in unpredictable patterns. Even after surgeons remove damaged tissue and stabilize circulation, the body can react in waves.
That’s what makes this moment so critical.
The Meaning of the “Golden Window”
In trauma recovery, a golden window is a decisive period when healing pathways either stabilize — or destabilize.
During this phase:
- Rebuilt tissue remains fragile
- Blood flow must remain steady
- Swelling must stay controlled
- Infection must be aggressively prevented
The ICU team worked through the night adjusting fluid balances carefully. Too little fluid risks organ strain. Too much can increase compartment pressures in already traumatized muscle groups.
Compartment pressure monitoring became a central focus.
If pressure builds beyond safe thresholds, circulation can become compromised — threatening tissue surgeons fought to preserve during earlier operations.
Why Muscle Spasms Matter
The intense muscle spasms Hunter experienced were not simply discomfort.
After high-voltage trauma and surgical intervention, spasms can indicate:
- Nerve irritation
- Electrolyte imbalance
- Tissue stress
- Inflammatory escalation
Uncontrolled spasms increase metabolic demand and strain oxygen delivery to recovering tissue. In a patient already navigating systemic stress, this becomes a serious variable.
The care team responded with medication adjustments, lab analysis, and repeated bedside evaluations to determine the trigger.
Protecting What Has Been Saved
Surgeons have already completed multiple procedures to remove damaged tissue and preserve viable muscle and circulation.
Now, the objective shifts:
Not repair.
Protection.
This stage is about maintaining stability long enough for the body’s natural healing processes to take hold.
That requires:
- Controlled inflammation
- Balanced electrolytes
- Stable blood pressure
- Adequate oxygenation
- Vigilant infection monitoring
Even minor delays in responding to abnormalities can widen complications quickly in electrical trauma cases.
That’s why every alarm matters.
ICU Vigilance Through the Night
Family members described the overnight hours as exhausting — but focused.
No panic.
Just relentless vigilance.
Nurses rotated continuously. Physicians reassessed trends. Labs were drawn repeatedly to monitor:
- White blood cell counts
- Lactate levels
- Kidney function
- Electrolyte balance
Circulation checks were performed at regular intervals to ensure no developing vascular compromise.
The goal is clear:
Stabilize.
Hold the line.
Prevent another emergency return to the operating room.
The Primary Trigger Behind the Red Alerts
Doctors have identified fluid imbalance — specifically rapid intravascular shifts — as the primary trigger behind last night’s red alerts.
When trauma patients retain or redistribute fluids too quickly, tissue compartments can swell, increasing pressure internally. That pressure can:
- Restrict blood flow
- Compromise oxygen delivery
- Increase risk of further tissue damage
The medical team is watching for a specific stabilization threshold today:
A sustained reduction in compartment pressures combined with normalized fluid balance markers.
If those two metrics stabilize, surgical intervention may be avoided.
If they trend upward again, operating room readiness remains in place.
Why Today Matters
Trauma recovery is not linear.
It’s measured in phases.
This golden window represents a pivot point. If Hunter’s fluid levels respond to adjustment and spasms settle under controlled medication, today could mark the beginning of stronger stabilization.
That would shift focus toward gradual healing rather than crisis response.
But if swelling escalates or infection markers rise, surgical teams are prepared to intervene immediately.
The line between those outcomes can be narrow.
The Emotional Weight
For Hunter’s family, the night carried emotional intensity — but not chaos.
They describe the environment as controlled, professional, determined.
They understand the stakes.
They also understand that survival in cases like this is often secured hour by hour — not day by day.
There are no guarantees.
Only vigilance.
What Comes Next
Throughout the day, doctors will monitor:
- Compartment pressure readings
- Fluid output trends
- Spasm frequency and severity
- Inflammatory markers
- Oxygenation stability
If trends improve, Hunter’s recovery narrative shifts toward consolidation and endurance.
If thresholds are crossed, another procedure could become necessary to relieve pressure or address emerging complications.
Right now, the objective remains the same:
Protect what has been rebuilt.
Prevent regression.
Secure stability.
Overnight alarms signaled risk.
Today will reveal whether intervention locked in progress — or whether the fight requires another round.
For now, Hunter remains under intensive monitoring.
Vitals guarded.
Teams prepared.
The golden window still open.
